Posted by Dr Michelle Wright
Meningitis
Meningitis – what causes it, a symptoms checklist to look out for, its treatment and what we can do to prevent it. The meninges is a protective lining which covers the brain and spinal cord. Meningitis happens if these meninges become inflamed. Bacteria, viruses and rarely fungal infections and tuberculosis can cause this inflammation.
Viral or bacterial meningitis?
Viral meningitis is the most common. It’s usually less serious, with most people recovering fully with no long-term problems. Bacterial meningitis is less common but is the one that is talked about the most in the media due to the serious nature of the illness that it causes. Most cases of bacterial meningitis are caused by the bacterium Neisseria meningitidis – also known as meningococcus. In Switzerland each year, around 60 severe cases of meningococcal meningitis are declared.
10-15% of the European population carry these bacteria in their nose and throat where it causes them no harm. These ‘carriers’ or an unwell person can pass on infection to others through intimate contact, coughing or sneezing.
Who is most at risk?
We don’t fully understand why the bacteria live harmlessly in the body of carriers but cause serious infection in others. People most at risk of developing meningococcal meningitis are the under 5s and then adolescents between the ages of 15 and 19.
Meningitis symptoms
In terms of meningitis symptoms, the classic ones to look out for in older children and adults are: high fever, headache, a stiff neck and photophobia – a dislike of bright lights. The person may also complain muscle and joint pains, appear drowsy or confused and start vomiting.
In babies, look for high fever with paradoxically cold hands and feet, excessive crying, fast breathing, difficulty feeding, drowsiness and irritability.
What about the rash?
With meningococcal meningitis, a typical rash is common. It usually starts as small red or purple spots that can develop anywhere on the body. The spots can get bigger and become blotchy, looking a bit like bruises.
The key thing about these spots is that they do not fade away when you press on them – they are non-blanching. Test for this using a clear glass tumbler. Press the side of the glass on the skin over some of the spots. Call for immediate medical help if you can still see the spots through the glass. Call 144 for an ambulance.
Septicaemia
But not everyone with meningitis develops a rash. As I mentioned, the rash is typical of meningococcal infection and usually indicates that the bacteria have entered the person’s blood stream and started to spread elsewhere in their body. We call this septicaemia.
When to seek urgent medical attention
Be alert to the symptoms and seek urgent medical attention if you are concerned. The sooner a person with meningitis is treated, the better their chance of full recovery.
Blood tests and a lumbar puncture (taking a sample of the fluid that bathes the brain and spinal cord at the base of the spine) can help to confirm the diagnosis of meningitis and look for the bacteria, virus or other bug that is causing the infection.
If bacterial meningitis is suspected, antibiotics are prescribed with the ‘best guess’ antibiotic being used until the full test results are back. As antibiotics don’t kill viruses, if it does turn out to be a viral meningitis, the antibiotics are stopped to leave the body’s own immune system to fight off the infection.
Vaccines
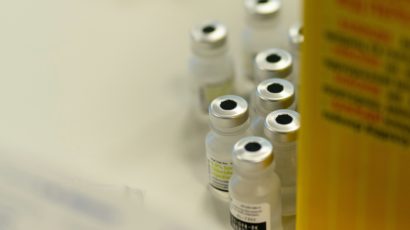
There are vaccines available to help protect against some of the causes of meningitis. Some are offered as part of the routine vaccination schedule in Switzerland and others as complementary vaccinations. Ask your paediatrician for more information.
Join one of our first aid courses designed with you and your family in mind. With babies and children and children in mind, this course enables you to act in the event of a medical emergency.